Why We Experience Inflammation
Our immune system evolved primarily to deal with infections, which were a leading cause of illness and death. As we now live much longer, our immune systems become activated to trigger chronic, low-grade inflammation. This then drives inflammatory and autoimmune diseases and degeneration of tissues in the brain and body as we age.
Systemic inflammation in the body can lead to musculoskeletal, lung, kidney, gut, skin, eye and other diseases. By blocking the initiation and/or progression of harmful inflammation in these conditions, we aim to treat both the symptoms and the underlying causes of illnesses that affect many people.
Increasing evidence also supports a pivotal role for chronic inflammation in the advent and progression of neurodegenerative diseases such as Parkinson’s and Alzheimer’s. Dysfunction of immune cells (microglia and astrocytes) in the brain leads to impaired clearance of toxins, such as amyloid, or can cause the immune system to aberrantly destroy cells essential for correct functioning of the brain.
Receptor X and complement factor B (FB) have been identified as key drivers of these processes and are implicated in a large number of diseases. At Sitala we are identifying and developing potent, best-in-class, small molecule Receptor X antagonists and FB inhibitors to stop inflammation before it gets out of control.
The Science of Harmful Inflammation
The immune system has multiple elements that enable it to fight infection and remove debris from our bodies. Immune cells use soluble ‘messenger’ molecules to communicate with each other and recruit additional cells to the site of inflammation. This is normally transient due to mechanisms that turn off inflammation and restore a normal state of balance in tissues once the infection is cleared.
In many chronic autoimmune and inflammatory diseases, signals that cause inflammation are overwhelming and cannot be controlled, leading to local tissue damage that can also spread to other parts of the body, such as the skin, eye and lungs.
Sitala’s strategy includes a broad approach to dampen the process that generates messenger molecules and a second, more precise approach to prevent messenger molecules from interacting with immune cells.

Complement
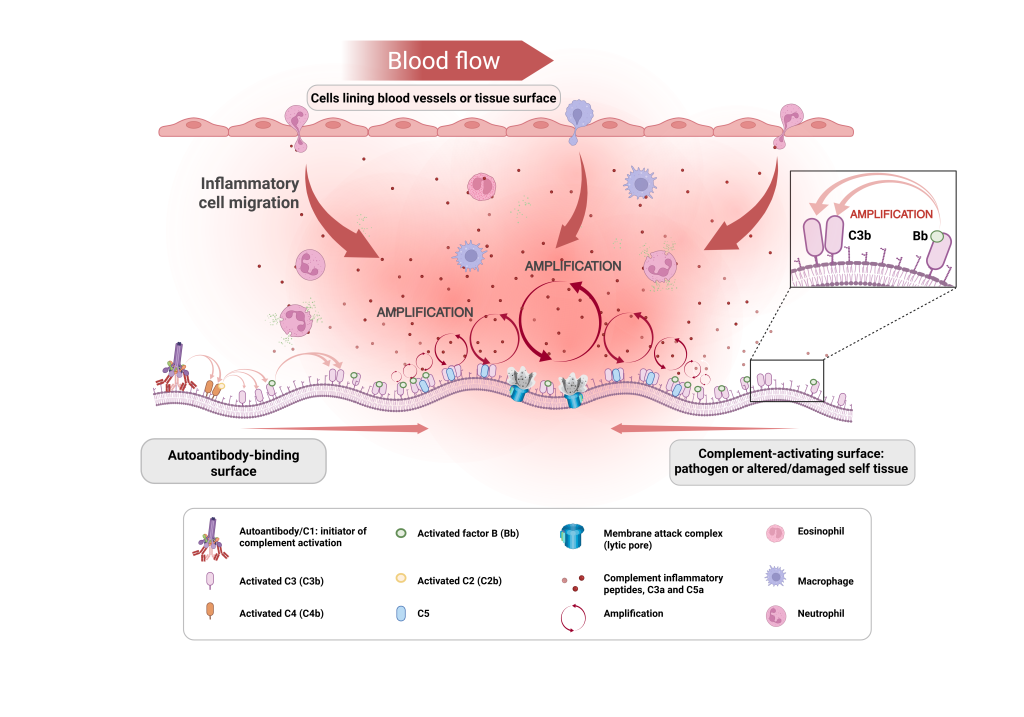
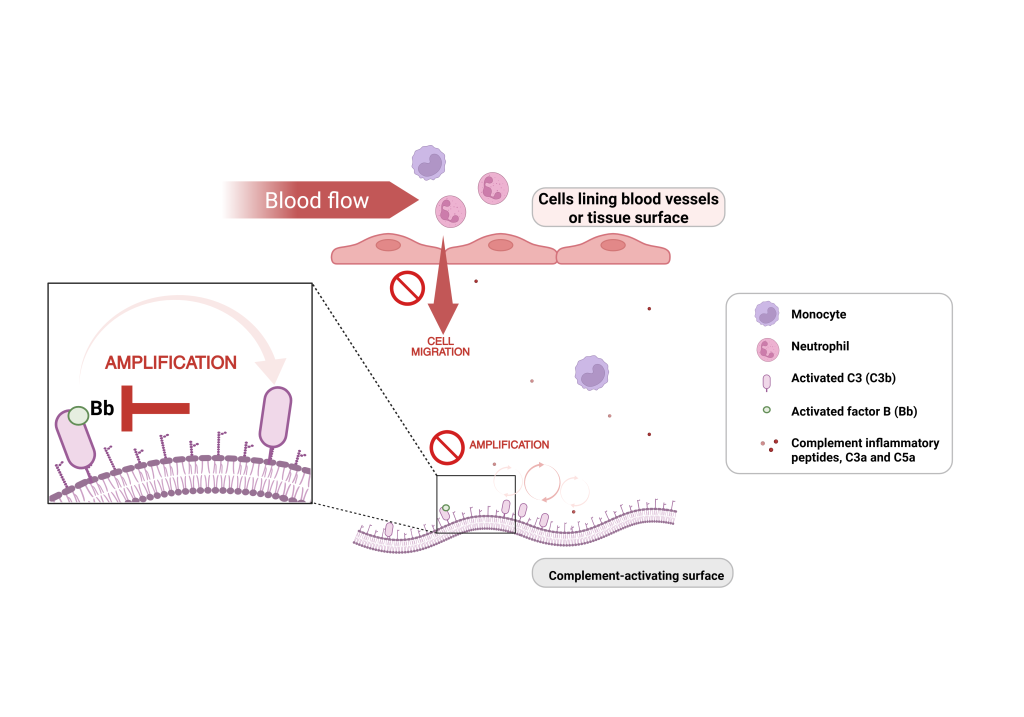
The complement cascade is an essential part of the innate immune system that constantly probes the environment for foreign substances, tissue debris and pathogens that need to be removed. Complement activation on the target surface coats it with fragments that ‘mark’ it for removal, while simultaneously generating small messenger proteins (such as C3a and C5a) that drift from the activating site and signal immune cells to migrate to the tissue and remove the pathogen or debris. Once a harmful substance is detected, a highly efficient mechanism kicks in that rapidly amplifies the cascade process. This generates an abundance of inflammatory mediators to attract and activate more immune cells. Activated factor B is a key driver of the amplification process. In some cases, membrane attack complexes (MAC) are assembled that punch holes through cell membranes to cause direct lysis and death. This results in the cell ‘exploding’, which further drives the cycle of inflammation.
This dysregulation can be managed early on with small molecule oral therapeutics that precisely block amplification or dampen the signalling to immune cells. This can help prevent the long-term effects of this harmful inflammation and slow or stop damage to organs such as the lungs, eye and skin.
Complement-Driven Autoinflammatory Diseases
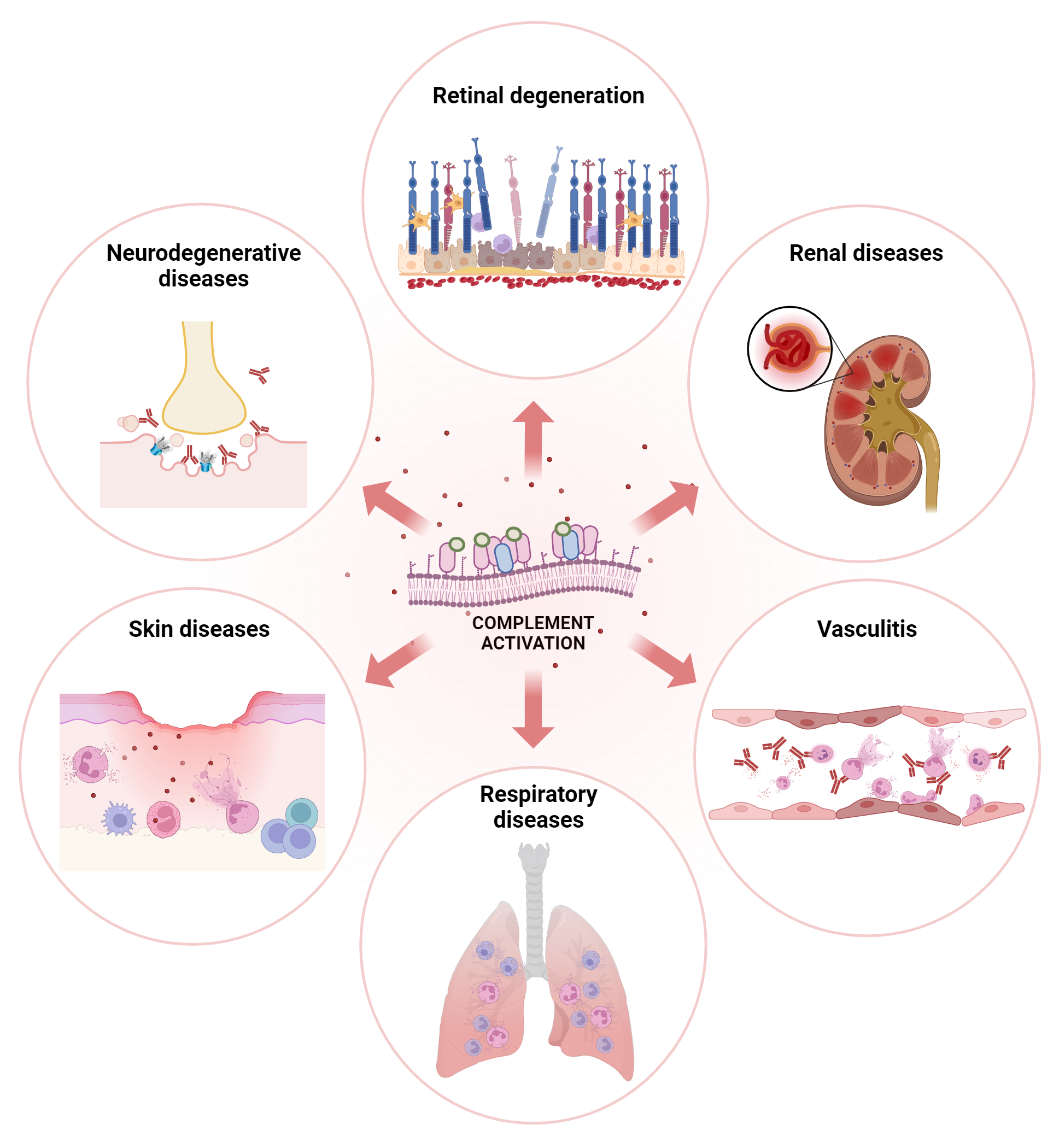
Diseases driven or exacerbated by complement are wide-ranging. Autoantibodies can bind inappropriately to cell surfaces, activating complement and damaging cell membranes. This can then directly affect the ability of nerves to function correctly in various neuropathies, or it can set up a localised skin inflammation that builds into a devastating and painful blistering condition.
Cellular immune mechanisms can trigger tissue damage, causing complement to activate and drive a vicious cycle of enhanced inflammation and further damage. In this way, a small trigger is amplified to a major downstream impact. These mechanisms are also linked to lung and some autoimmune and inflammatory diseases.
Finally, inherited genetic traits that over-activate complement or impair the body’s ability to control complement can cause inflammation in organs, such as the kidney and eye, that are sensitive to complement dysregulation.
Discover more about our science
Our Patients
Coming soon
Contact us
Collaborating with Sitala offers an opportunity to be part of cutting-edge science that could transform the lives of patients worldwide. We welcome partnering interest from academia, biotech and pharma. We also welcome career enquires from motivated individuals looking to work in a dynamic and fast-moving, small team environment.